Contraception: Find a Method That Fits Your Life
Want reliable birth control without guesswork? Contraception isn’t one-size-fits-all. This page helps you compare real options, spot common side effects, and make choices that match your health, goals, and daily routine.
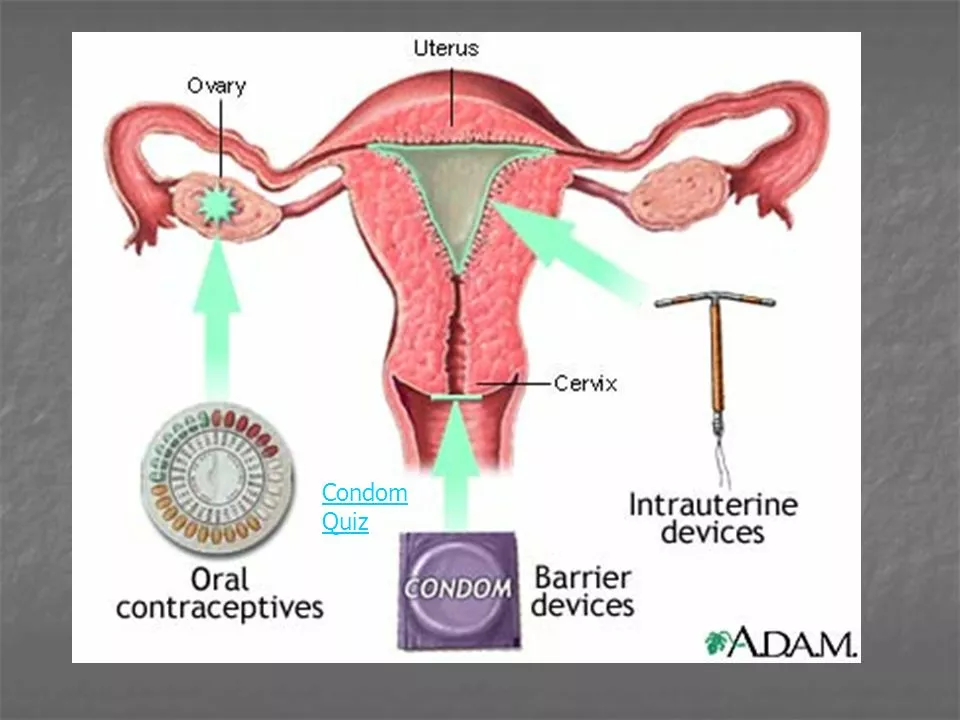
Short-acting methods are easy to start and stop. Pills, patches, and rings let you control timing and are reversible within weeks. They work well if you remember daily or weekly dosing. Condoms are short-acting too, and they’re the only method that also protects against STIs.
Long-acting reversible contraception (LARC) includes IUDs and implants. Once placed, they protect for years and remove the need to remember a daily pill. LARCs are highly effective and low-maintenance, but they require a clinic visit to insert and remove.
Permanent methods like tubal ligation or vasectomy are for people who are sure they don’t want future pregnancies. These are surgical choices and need a careful conversation with your doctor.
How to pick the right method
Start by asking three simple questions: Do you want kids soon? How reliable do you need it to be? Do you have any health issues—like migraines, blood clots, or high blood pressure—that affect your options? Your answers narrow the field fast.
If you want pregnancy in the near future, go with short-acting methods. If you want low maintenance and top effectiveness, LARCs are smart. If you need STD protection, use condoms along with another method.
Side effects matter and vary by method. Hormonal methods can cause nausea, mood changes, spotting, or breast tenderness. Copper IUDs may increase cramps or heavier periods for some people. Track side effects for a few months—many settle down, but persistent or severe symptoms need a doctor’s advice.
Emergency contraception and safety
Emergency contraception (EC) works after unprotected sex. Pills with levonorgestrel (Plan B-type) work best within 72 hours; ulipristal acetate (ella) works a bit longer. A copper IUD is the most effective EC if inserted within five days. EC doesn’t replace regular birth control and won’t cause long-term fertility problems.
Getting contraception: many methods need a prescription or clinic visit. If you consider buying online, stick to licensed providers and check reviews. Be cautious of sites that sell prescription meds without a proper consultation—safe care matters more than a quick price.
Practical tips: set phone reminders for pills, carry condoms, schedule IUD/implant checks after insertion, and keep a list of your meds to avoid interactions. Talk openly with your provider about side effects, sexual health, and future family plans.
If you’re unsure, a short telehealth visit can clarify options and prescriptions. If you experience heavy bleeding, severe abdominal pain, or sudden vision changes after starting a method, see a clinician right away.
Contraception should make life easier, not harder. Pick a method that fits your health and your routine, and don’t hesitate to switch if it doesn’t work for you.
The Connection between Contraception and Cancer Risk
In my recent research, I discovered a fascinating connection between contraception and cancer risk. It seems that certain types of contraceptives, such as hormonal birth control, may have both positive and negative effects on our cancer risk. On one hand, these contraceptives can lower the risk of ovarian and endometrial cancer, which is great news. However, there is also evidence suggesting that using these contraceptives may slightly increase the risk of breast and cervical cancer. As a blogger, I think it's crucial to keep exploring this topic and raise awareness about the benefits and risks associated with different contraceptive methods.
read more



