Stomach ulcers: what they are and what to do now
Waking with a burning ache in the upper belly or getting pain a few hours after eating? That can be a stomach (peptic) ulcer. A peptic ulcer is a sore in the stomach lining or the first part of the small intestine. They’re common, treatable, and often caused by things you can change or treat with medicine.
What usually causes stomach ulcers
Two things cause most ulcers: infection with H. pylori bacteria and long-term use of NSAID painkillers (like ibuprofen). Smoking makes ulcers worse and slows healing. Heavy alcohol, frequent heartburn, and stress can make symptoms worse but don’t usually cause ulcers by themselves.
Ulcers can appear in the stomach (gastric ulcer) or the duodenum (duodenal ulcer). The exact cause matters because it decides the treatment. For example, H. pylori needs antibiotics; NSAID-related ulcers need stopping or changing that medicine.
Common signs to watch for
Typical signs include a burning or gnawing pain between the breastbone and belly button, often worse when the stomach is empty. Other clues: nausea, bloating, burping, loss of appetite, and unintended weight loss. If you see blood in vomit or black, tarry stools, get medical help right away—those are warning signs of bleeding.
Your doctor will usually check for H. pylori with a breath or stool test. If symptoms are severe or tests are unclear, an endoscopy (a quick camera exam) may be done to look at the ulcer directly.
Treatment depends on the cause. If H. pylori is found, you’ll get a short course of antibiotics plus a proton pump inhibitor (PPI) to reduce acid and help healing. If NSAIDs caused the ulcer, stopping or switching the painkiller and starting a PPI is common. Some people at high risk may use protective drugs like misoprostol—but that’s prescription-only and has side effects, so discuss it with your clinician.
Over-the-counter antacids can ease pain briefly, but they don’t heal ulcers. PPIs (prescription or OTC versions) reduce acid and let the lining repair. Always finish the full treatment your doctor prescribes—stopping early increases the chance the ulcer returns.
Simple habits help healing: stop smoking, cut back on alcohol, avoid regular NSAID use, eat smaller meals, and don’t lie down right after eating. Stress management and regular sleep can ease symptoms, too.
If you have new, severe belly pain, black stools, fainting, or repeated vomiting, seek urgent care. For ongoing or mild symptoms, book a GP visit to test for H. pylori and get the right medicine. Fixing the cause usually fixes the ulcer—and most people recover well with the right care.
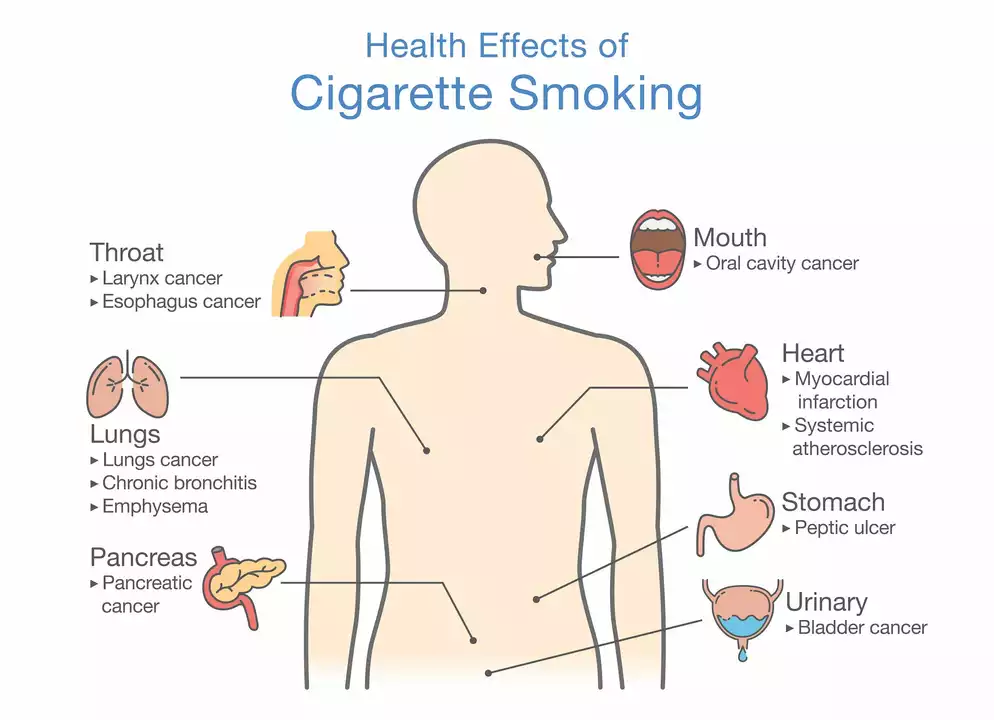
How Smoking Affects Your Risk of Developing Stomach Ulcers
As a blogger, I've been researching how smoking can affect our risk of developing stomach ulcers. I discovered that smoking greatly increases this risk, as it weakens the protective lining of our stomach, making it more susceptible to harmful stomach acids. Additionally, smoking hinders the healing process of existing ulcers, and may even cause them to recur. It's important for us to be aware of these risks and consider quitting smoking to maintain a healthy stomach. So, let's work on kicking this harmful habit to reduce the chances of developing painful stomach ulcers!
read more