Hormonal methods: pick the right hormonal birth control and therapy
Want reliable birth control or hormone treatment but confused by all the options? Hormonal methods work by changing your body's hormones to prevent pregnancy or manage conditions like menopause, acne, endometriosis, and some mood problems. This page gives clear comparisons, real risks, and practical safety tips so you can talk to your clinician with confidence.
Types of hormonal methods and how they work
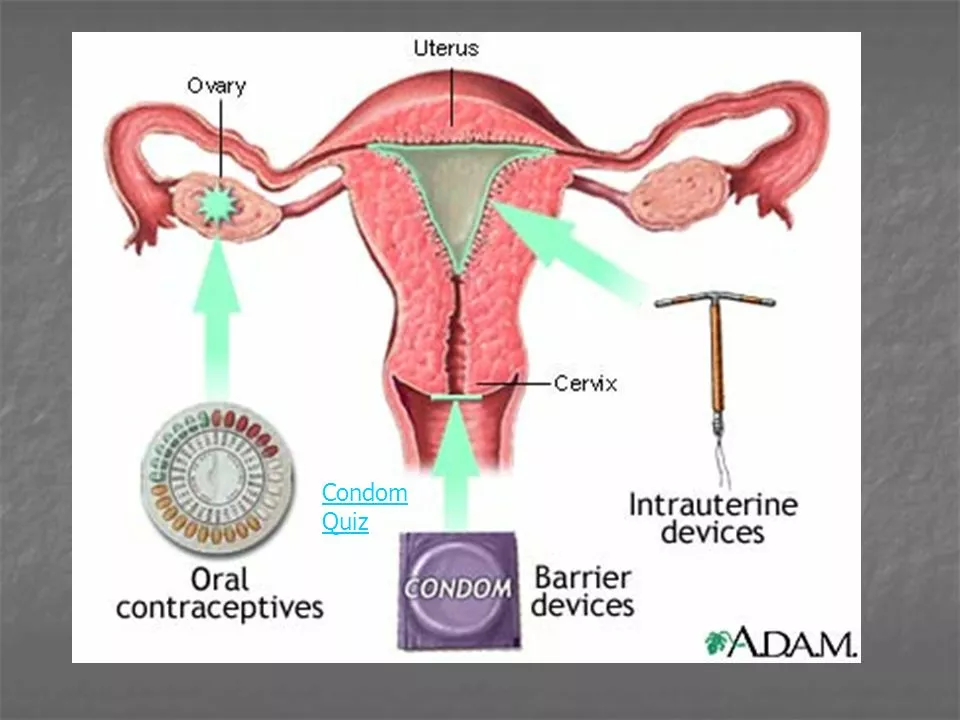
Pills, patches, rings, injections, implants, and hormonal IUDs are the common contraceptives. Most combine estrogen and progestin or use progestin alone. They stop ovulation, thicken cervical mucus, or thin the uterine lining so an egg can't implant.
- Combined pill/patch/ring: Daily pill, weekly patch, or monthly ring. Good for regular cycles and lighter periods.
- Progestin-only pill (mini-pill): For people who can’t take estrogen, including breastfeeding parents.
- Injectable (Depo): Shot every 3 months—low maintenance but can affect bone density with long use.
- Implant: Small rod under the arm that lasts 3–5 years. Very effective and reversible.
- Hormonal IUD: Placed in the uterus for 3–8 years. Great for heavy periods and long-term control.
Hormone therapy (HRT) for menopause or low hormone states uses similar hormones but at different doses and goals: relieve hot flashes, protect bones, or address mood and sexual changes. Your doctor tailors the type and dose to your symptoms and risks.
How to choose, side effects, and safety tips
Pick a method based on your health, how long you want protection, and side effects you can accept. If you smoke and are over 35, avoid estrogen-containing methods because of higher clot risk. If you plan pregnancy soon, choose short-acting options like pills or rings. Implants and IUDs work best when you want long-term, low-maintenance protection.
Common side effects include spotting, mood shifts, breast tenderness, and changes in libido. Serious but rare risks include blood clots (more with estrogen), high blood pressure, and certain interactions with other drugs. Enzyme-inducing medicines—some anti-seizure drugs and St. John’s Wort—can lower hormonal method effectiveness. Tell your clinician about all medicines and supplements you take.
Want to buy prescriptions online? Be careful. Use licensed pharmacies, require a real prescription, and check reviews. Our site has straightforward guides on safe online pharmacies and how to confirm legitimacy before you buy. Always confirm treatment with a healthcare provider rather than self-prescribing.
If you have unexplained heavy bleeding, chest pain, shortness of breath, sudden severe headache, or leg swelling, seek care right away. For routine questions—side effects, switching methods, or combining treatments—book a visit with your clinician or a telehealth service that checks your history and blood pressure before changing hormones.
Want a quick next step? Make a short list of your priorities (pregnancy plans, frequency of use, tolerance for side effects) and bring it to your appointment. Clear choices start with clear questions.
The Connection between Contraception and Cancer Risk
In my recent research, I discovered a fascinating connection between contraception and cancer risk. It seems that certain types of contraceptives, such as hormonal birth control, may have both positive and negative effects on our cancer risk. On one hand, these contraceptives can lower the risk of ovarian and endometrial cancer, which is great news. However, there is also evidence suggesting that using these contraceptives may slightly increase the risk of breast and cervical cancer. As a blogger, I think it's crucial to keep exploring this topic and raise awareness about the benefits and risks associated with different contraceptive methods.
read more



