Diverticulitis: Spotting a Flare and What You Can Do Now
Diverticulitis happens when small pouches in the colon (diverticula) get inflamed or infected. It can start like mild belly pain and end up needing a hospital visit — so knowing the signs matters. Below you’ll find simple, practical steps for recognizing symptoms, safe home care when appropriate, and clear reasons to call your doctor or head to the ER.
Symptoms and when to seek help
Typical signs are steady pain on the lower left side of the belly, fever, chills, nausea, and changes in bowel habits. If pain is severe, you have a high fever, vomiting you can’t control, blood in your stool, or trouble breathing, get urgent medical help. If symptoms are mild—low fever, mild pain—you can call your provider for advice and often manage at home with follow-up.
Older adults and people with weakened immune systems can get sicker fast. Don’t try to tough it out if you fall into those groups; early evaluation cuts risk of complications.
Treatment, diet and prevention
Mild cases are commonly treated with rest, clear liquids or a low-fiber diet for a short time, and sometimes oral antibiotics. Your doctor will tell you what’s best based on exam and tests. Severe cases can require IV antibiotics, a hospital stay, drainage of an abscess, or rarely, surgery.
Diet advice often changes with the stage: during a flare, many doctors recommend a short period of low-fiber foods or liquids to rest the gut. Once recovery starts, slowly increase fiber through foods like oats, beans, fruits, and vegetables. High-fiber diets and regular fluids help stool move more smoothly and reduce pressure in the colon, which lowers the chance of future flares.
You may have heard to avoid nuts, seeds, or popcorn. Recent research shows those foods don’t clearly raise risk of attacks, so focus on overall fiber and bowel regularity instead of strict bans. If a specific food seems to trigger your symptoms, talk with your doctor or dietitian.
Other practical tips: stay active, maintain a healthy weight, and avoid smoking. If you have repeated severe attacks or complications like fistulas or strictures, surgery to remove the affected segment may be recommended.
Keep a symptom log — note what you eat, pain levels, bowel changes, and any medicines. That record helps your provider make treatment decisions faster. If you’re unsure, call your clinic; early treatment usually means simpler care and fewer complications.
If you want to read more detailed articles—like diet guides, when surgery is needed, or how antibiotics are chosen—check the related posts on KiwiDrug.com or message your healthcare team for advice tailored to you.
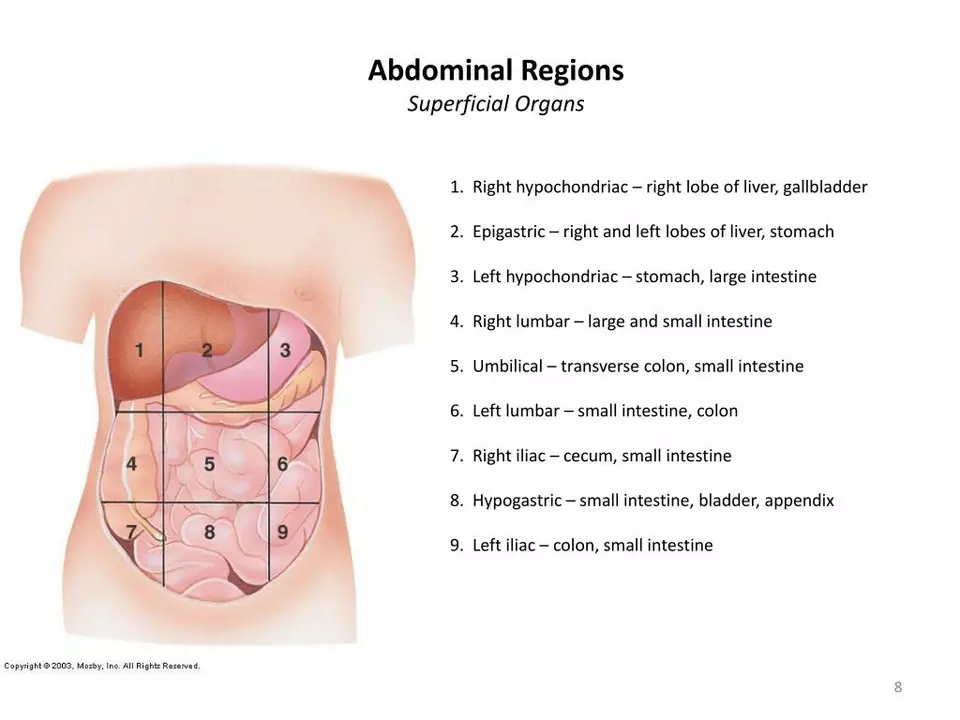
Epigastric Pain and Diverticulitis: Understanding the Connection
As a blogger who's been researching the connection between epigastric pain and diverticulitis, I've found some interesting insights to share. First, epigastric pain is the discomfort felt in the upper abdomen, usually in the middle, while diverticulitis is the inflammation of small pouches called diverticula in the digestive tract. Although they may seem unrelated, there is indeed a connection between the two. In some cases, diverticulitis can cause epigastric pain as a result of the inflammation spreading to nearby tissues, leading to abdominal discomfort. It's essential to consult with a healthcare professional if you experience persistent epigastric pain, as it could be a sign of diverticulitis or other underlying issues.
read more