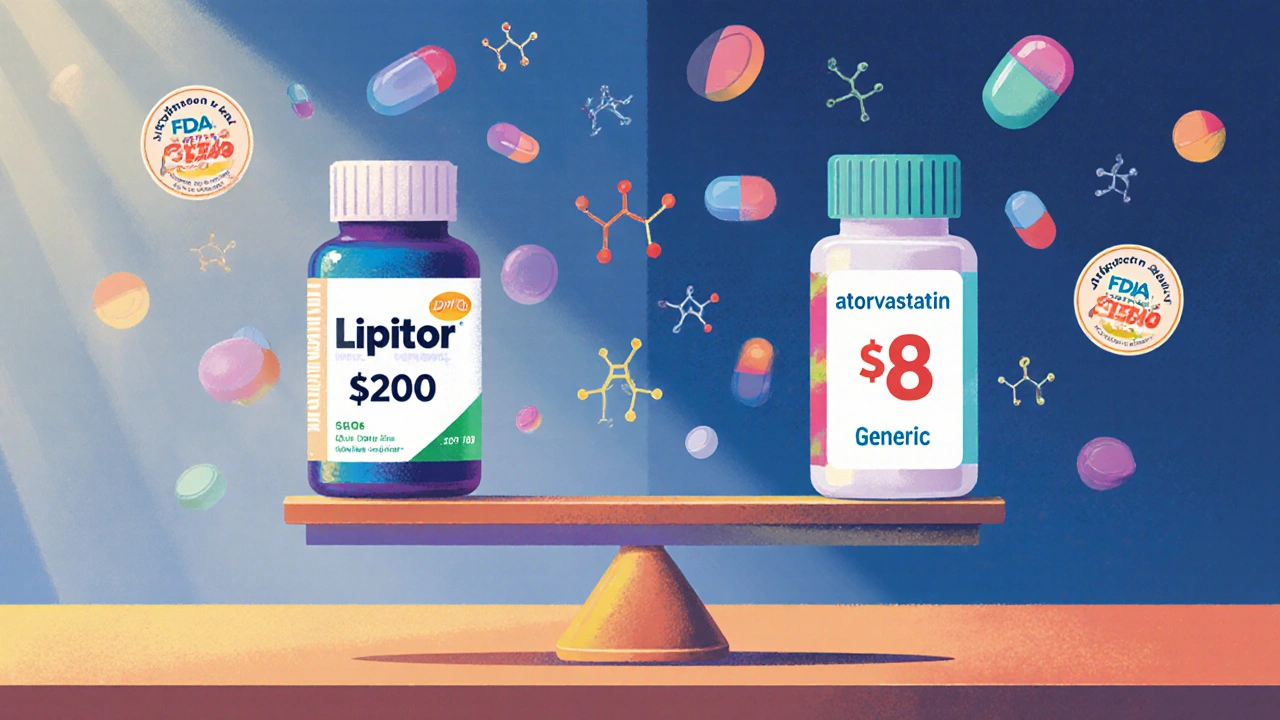
When you pick up a prescription, you might see two options on the receipt: the name you recognize, like Lipitor, and a simpler one, like atorvastatin. The first is the brand-name drug. The second is the generic. They do the same thing. But one costs a fraction of the other. Why? And should you care?
What Exactly Is a Generic Drug?
A generic drug isn’t a copy. It’s not a cheaper version. It’s the exact same medicine. Same active ingredient. Same dose. Same way it works in your body. The FDA requires generics to match brand-name drugs in strength, purity, stability, and how quickly they’re absorbed. That’s not a guess - it’s a strict test called bioequivalence. The generic must deliver the same amount of drug into your bloodstream within 80-125% of the brand’s performance. If it doesn’t pass, it doesn’t get approved.
Generics become available after the brand-name drug’s patent expires. That’s usually 10-12 years after launch. Once that happens, other companies can make it. They don’t have to repeat expensive clinical trials. They just prove they match the original. That’s why they’re cheaper. Not because they’re lower quality. Because they skip the R&D costs.
How Much Do Generic Drugs Actually Save You?
The numbers are staggering. In 2024, generic drugs made up 90% of all prescriptions filled in the U.S. But they cost only 12% of what brand-name drugs did. That means for every $100 spent on prescriptions, $88 went to brand-name drugs - even though they were used in just 1 out of every 10 fills.
On average, generics cost 79-85% less than their brand-name counterparts. Take atorvastatin (Lipitor). The brand version can run over $200 for a 30-day supply. The generic? Often under $10 - sometimes even free with insurance. That’s not a small difference. That’s life-changing for people on fixed incomes.
And it’s not just one drug. In markets with just one generic competitor, prices drop to about 90% of the brand’s price. With three or four generics, prices fall to 60-70%. With five or more? They drop below 50%. The more competition, the lower the price. That’s how free markets work - and it’s why generic drugs are the only part of healthcare spending that consistently goes down.
Why Do Brand-Name Drugs Still Cost So Much?
It’s not because they’re better. It’s because they’re protected. Patents give companies a monopoly. During that time, they set high prices to recoup research costs - and make profits. But once generics enter, something interesting happens.
Some brand-name companies lower their prices before generics even launch. Bayer cut the list price of Nexavar by 50% in 2025 after the first generic version came out. Merck dropped Januvia prices by 42.4%. Why? Because they know they can’t compete on price. So they try to stay relevant by lowering costs before the market crushes them.
There’s another twist: list price vs. net price. The price you see on a billboard or in an ad? That’s the list price. The actual price paid after rebates, discounts, and insurance negotiations? That’s the net price. In 2024, brand-name list prices rose slightly, but net prices barely moved. That’s because manufacturers are giving bigger discounts to insurers and pharmacies to stay on formularies. So while the sticker price looks high, what you pay out-of-pocket might not be as bad - unless you’re uninsured or paying cash.

Do Generics Work as Well as Brand-Name Drugs?
Yes. Absolutely.
The FDA, the American Medical Association, and every major medical group agree: generics are therapeutically equivalent. They’re not “good enough.” They’re the same. A 2025 Tebra survey found 84% of Americans believe generics are just as effective. But here’s the catch: 62% still trust brand-name drugs more. Why? Because of perception, not science.
People think, “If it’s cheaper, it must be worse.” That’s not true. Generics use the same active ingredients. They’re made in the same kind of facilities. They’re held to the same standards. The only differences are in the inactive ingredients - things like fillers, dyes, or coatings. These don’t affect how the drug works. They just change the pill’s shape or color.
Some people report feeling different on a generic. That’s usually because the pill looks different. Or because they’re used to the brand. But if you switch from Lipitor to atorvastatin and feel worse, it’s likely not the drug. It’s your brain.
Why Don’t More People Choose Generics?
Cost isn’t the only barrier. Perception is.
Even though 63% of Americans choose generics because of price, 60% say they’d prefer the brand if they could afford it. That’s a big gap between what people know and what they do. It’s also why pharmacies sometimes don’t automatically switch you to generics - unless you ask.
Some doctors still prescribe by brand name out of habit. Or because they’re unsure about patient trust. But that’s changing. More physicians now write “dispense as written” only if there’s a real reason not to use the generic. Otherwise, they let the pharmacist substitute.
And here’s something most people don’t realize: if you’re on Medicare, the Inflation Reduction Act will cap your out-of-pocket drug costs at $2,000 per year starting in 2026. That could push even more people toward generics - because they’re the easiest way to stay under the cap.

When Should You Avoid Generics?
Almost never. But there are rare exceptions.
Some drugs have a narrow therapeutic index - meaning the difference between a safe dose and a harmful one is very small. Examples include warfarin (a blood thinner), levothyroxine (for thyroid), and phenytoin (for seizures). For these, small differences in absorption could matter.
That’s why doctors sometimes ask patients to stick with one brand. But even here, switching between generics is usually safe. The key is consistency. If you start on a generic, stay on it. Don’t keep switching between different generic brands unless your doctor says it’s okay.
Also, some older drugs don’t have generics because no company has bothered to make them. Or because the market is too small. But those are the exception, not the rule.
How to Get the Best Deal on Your Prescriptions
Here’s how to save money without sacrificing quality:
- Ask your doctor if a generic is available. Don’t assume they know - ask.
- Ask your pharmacist to switch you to the generic if you’re on a brand. Most pharmacies will do it automatically unless you say no.
- Use pharmacy discount cards. GoodRx, Blink Health, and others often list generics for under $5 - even without insurance.
- Check your Medicare Part D plan. Some plans have lower copays for generics. You might be able to switch plans during open enrollment.
- Buy in bulk. Many generics cost less per pill when you get a 90-day supply instead of 30.
And if you’re paying cash? Always ask for the cash price. Sometimes it’s cheaper than your insurance copay.
The Bigger Picture: Why This Matters
Generic drugs aren’t just about saving money on a single prescription. They’re about keeping the whole system running. In 2024, Americans spent $98 billion on generics - and saved over $6.4 billion compared to what they would’ve spent on brands. That’s money that goes back into people’s pockets, into small businesses, into food, rent, and healthcare for other needs.
The U.S. spends more on drugs than any other country - but only because of brand-name prices. When you look at total prescription spending, the U.S. actually has lower net prices than Canada, Germany, and the UK. Why? Because of generics. They’re the hidden engine of affordability.
High brand prices fund innovation. Low generic prices make sure everyone can afford treatment. It’s a system that works - if you use it right.
So next time you see a generic option, don’t think “cheap.” Think “smart.”
Are generic drugs really as effective as brand-name drugs?
Yes. Generic drugs contain the same active ingredients, work the same way, and meet the same strict standards as brand-name drugs. The FDA requires them to prove bioequivalence - meaning they deliver the same amount of medicine into your bloodstream at the same rate. Thousands of studies confirm they work just as well.
Why are generic drugs so much cheaper?
Generic manufacturers don’t have to pay for expensive clinical trials or marketing campaigns. Once a brand’s patent expires, other companies can produce the same drug by proving it’s bioequivalent. That cuts costs dramatically. The savings are passed on to consumers - not because the drug is inferior, but because competition drives prices down.
Can I switch from a brand-name drug to a generic safely?
For most medications, yes. Your pharmacist can substitute a generic unless your doctor writes “dispense as written.” If you’re on a drug with a narrow therapeutic index - like warfarin or levothyroxine - talk to your doctor first. But even then, switching between generics is usually safe as long as you stick with one brand.
Do generic drugs have the same side effects?
Yes. Since they contain the same active ingredient, the side effects are identical. Differences in inactive ingredients (like dyes or fillers) might cause rare allergic reactions, but those are uncommon and unrelated to effectiveness. If you notice new side effects after switching, tell your doctor - but don’t assume it’s the generic’s fault.
Why do some people say generics don’t work for them?
Often, it’s psychological. People associate the look, size, or color of the pill with the brand. If the generic looks different, they feel like it’s not working - even if it’s chemically identical. In rare cases, switching between different generic brands can cause slight variations in absorption, which is why consistency matters. But for most people, the effect is the same.
How do I know if my prescription has a generic version?
Ask your pharmacist. Or search the drug’s generic name online - most brand-name drugs have a generic by now. For example, if you’re on Crestor, the generic is rosuvastatin. If your doctor prescribed a brand, ask if a generic is available. Many insurance plans require you to try the generic first.
Will Medicare cover generics?
Yes. Medicare Part D plans cover most generics, often with lower copays than brand-name drugs. Starting in 2026, the out-of-pocket cap for all drugs - brand or generic - will be $2,000 per year. Generics make it easier to stay under that limit.
Are all generic drugs made in the U.S.?
No. Many generic drugs are manufactured in countries like India and China. But every facility - whether in the U.S., India, or elsewhere - must meet FDA standards. The FDA inspects these facilities regularly. If a plant fails inspection, its drugs are blocked from entering the U.S. market.
Can I trust online pharmacies that sell generics?
Only if they’re verified. Look for the VIPPS seal (Verified Internet Pharmacy Practice Sites) or check the FDA’s list of approved online pharmacies. Many websites sell fake or contaminated drugs. Stick to reputable pharmacies - even if the price is a little higher. Your health isn’t worth the risk.
What’s the future of generic drug pricing?
Prices will keep falling as more generics enter the market. But some manufacturers are using value-based pricing - lowering brand prices before generics launch to stay competitive. Meanwhile, Medicare’s new price negotiation rules and the $2,000 out-of-pocket cap will push even more people toward generics. The trend is clear: generics are becoming the default - not the backup.
Generics are not a compromise. They’re the smart choice. They’re proven. They’re safe. And they save billions every year. If your doctor prescribes a brand, ask: “Is there a generic?” You might be surprised by the answer - and the savings.






12 Comments
Oh wow, a 90% generic market share and you're still surprised people don't trust them? 😂 Maybe because Big Pharma spent $20 billion convincing us that blue pills are somehow *more* medicine than white ones. I mean, if your doctor prescribes Lipitor and you get atorvastatin, do you at least get a free therapist to cope with the existential crisis of your pill looking different?
I switched to generic levothyroxine last year and my TSH went wild. My doctor said it was 'probably coincidence' but I'm not taking the risk again. I know it's irrational, but I need to feel like I'm getting the real thing. Even if it costs half my rent.
Y'all, I just want to hug whoever wrote this. 🤗 I’m a single mom in Lagos and my son’s asthma inhaler used to cost me a week’s groceries. When we switched to the generic? I cried. Not because I was sad - because I could finally breathe without my heart breaking. Generics aren’t just cheaper - they’re dignity. And yeah, the pill looks different. But my baby’s lungs don’t care what color it is. 💙
Generics are the quiet heroes of healthcare. 🤫 We don’t cheer for them like we do for new drugs with flashy ads, but without them, millions would just… not take their meds. It’s not just about money - it’s about access. And access is a human right. I’m grateful for the scientists who made generics possible, the pharmacists who recommend them, and the people who just… take them. 🙏
My pharmacy automatically switches me to generics - and I never even noticed. I just know my blood pressure’s stable and my wallet’s happy. 😊 If you’re nervous about switching, talk to your pharmacist. They’re the real MVPs here.
If you're still using brand-name drugs because you 'trust' them, you're either rich or gullible. The FDA doesn't play games. Your 'brand loyalty' is a marketing scam. Stop being a sucker and save your money. Your future self will thank you.
So I got my generic warfarin last month. The pill’s a different shape, different color, no logo - just ‘5 mg’ stamped on it. I stared at it for 10 minutes. Then I took it. Then I Googled ‘can generic warfarin kill you’ - spoiler: yes, but so can the brand if you miss a dose. I’ve been on it for 6 months now. Still alive. Still not scared. But I still check the label. Every. Single. Time. 🤷♂️
One of my patients switched from brand-name Januvia to generic sitagliptin and said, ‘I feel like I got a raise.’ That’s the kind of win we need more of. Generics aren’t second-rate - they’re second-to-none. Keep asking, keep switching, keep saving. You’ve got this!
It’s fascinating how perception overrides evidence here. We accept that a generic iPhone charger works fine, but a generic pill? ‘It’s not the same!’ Why? Because we’ve been conditioned to equate price with value - even when the chemistry says otherwise. The real crisis isn’t drug cost - it’s our collective trust deficit. We’ve been taught to fear the cheap, even when it’s identical. That’s not science. That’s propaganda.
Look, I’m not some peasant. I pay for quality. Why would I risk my health on some Indian-made pill with no brand? If you can’t afford the real thing, maybe you shouldn’t be taking it at all.
It is an undeniable fact that the United States of America leads the world in pharmaceutical innovation, and any attempt to equate domestically manufactured brand-name medications with foreign-produced generics is not only scientifically inaccurate but also a direct affront to American exceptionalism. The FDA's standards, while nominally equal, are not applied with the same rigor abroad. The foreign manufacturing of generics constitutes a national security vulnerability. We must prioritize American-made medicine - or risk the erosion of public health integrity.
You know what’s wild? I used to think generics were sketchy. Then I started working at a pharmacy. I’ve seen the same factory that makes Lipitor also make atorvastatin - same machines, same line, same quality control. The only difference? The label. And the price tag. I’ve watched people cry when they find out their $200 pill is the same as the $8 one. It’s not about science. It’s about branding. And honestly? That’s the saddest part. We’re paying for a logo. Not medicine. Just… a logo.