Cancer Risk: Practical Ways to Understand and Reduce It
Fact: about one-third of cancers are linked to lifestyle and infections — so some risks are in your control. This page helps you spot the biggest risk factors, pick simple actions you can take, and know when to talk to a doctor.
Smoking is the single biggest preventable cause of cancer. Quitting cuts your risk for lung, throat, and several other cancers. If you smoke, ask your doctor about nicotine replacement, prescription medicines, or local quit programs. Even cutting back helps while you build toward quitting entirely.
Alcohol raises the risk for breast, liver, mouth, and esophageal cancers. Keep intake low: for most people that means no more than one drink a day for women and two for men. If you drink heavily, a plan to reduce or stop drinking lowers your risk quickly for several health problems.
Body weight and activity matter. Excess body fat links to cancers of the bowel, breast (post-menopause), endometrium, and pancreas. Aim for regular movement, strength work twice a week, and a balanced diet high in vegetables, whole grains, and modest in processed foods and red meat.
Some infections increase cancer risk. HPV causes cervical and some throat cancers; HPV vaccination prevents most of these. Hepatitis B and C raise liver cancer risk — vaccination and testing can help. Good hygiene, safe sex, and vaccination are clear ways to reduce infection-related cancer risk.
Sun and tanning bed exposure causes skin cancers, including melanoma. Use sunscreen with SPF 30+, wear protective clothing, and skip indoor tanning. Check your skin monthly and see a dermatologist for any spot that changes, itches, or bleeds.
Know your family history. Some cancers run in families due to inherited genes. If several close relatives had early-onset cancer, ask about genetic counseling and testing. Results can change screening plans and preventive steps.
Work and environment matter too. Some jobs expose you to chemicals or radiation that raise cancer risk. Use protective equipment, follow safety rules, and raise concerns with your workplace health officer. For household hazards, test for radon and follow local guidance if levels are high.
Screening saves lives. Talk to your doctor about breast, cervical, colon, and lung screening based on age, smoking history, and other risks. Screening finds some cancers early when treatment is simpler and outcomes are better.
Medications and special cases
Certain medicines and medical treatments can change cancer risk. If you take long-term drugs or cancer therapies like targeted agents, keep up with follow-up care and report new symptoms. Articles on this site cover drug interactions and treatment monitoring — useful if you’re on medicines such as alpelisib or ibrutinib.
Practical next steps
Make a short checklist: quit or cut back on smoking and alcohol, move 150 minutes a week, get vaccinated (HPV, Hep B), follow screening guidelines, and discuss family history with your clinician. Small, steady changes add up. If you’re worried about symptoms or your personal risk, book a medical review — early action gives you options.
Start with one change this week and track your progress.
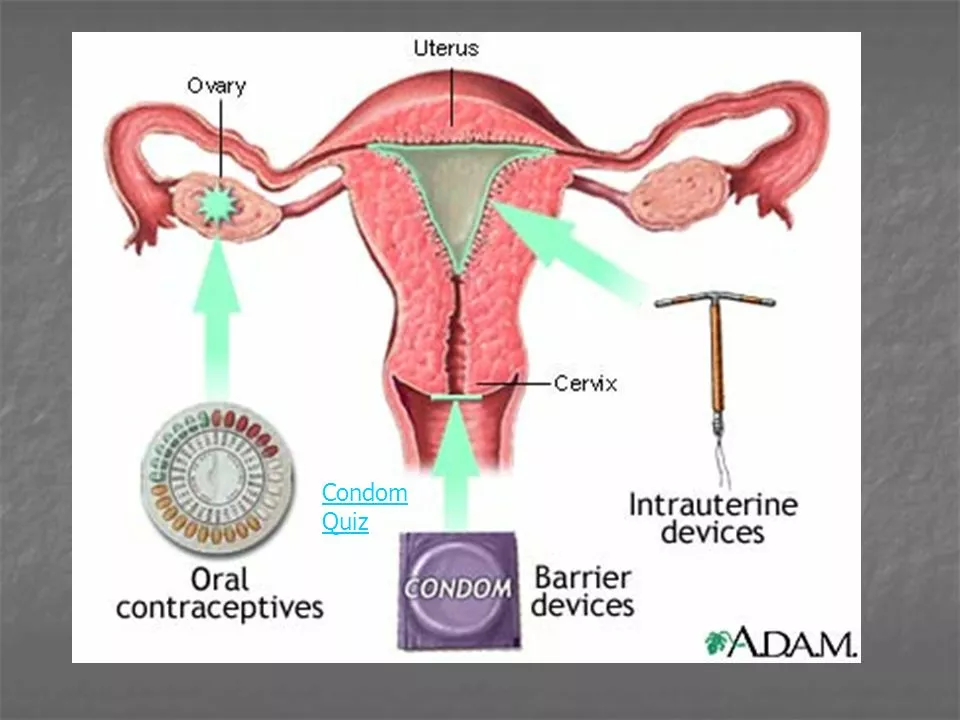
The Connection between Contraception and Cancer Risk
In my recent research, I discovered a fascinating connection between contraception and cancer risk. It seems that certain types of contraceptives, such as hormonal birth control, may have both positive and negative effects on our cancer risk. On one hand, these contraceptives can lower the risk of ovarian and endometrial cancer, which is great news. However, there is also evidence suggesting that using these contraceptives may slightly increase the risk of breast and cervical cancer. As a blogger, I think it's crucial to keep exploring this topic and raise awareness about the benefits and risks associated with different contraceptive methods.
read more



